
Prenatal, Birth & Postpartum Care where you are heard, supported, and truly valued. Because it’s essential.
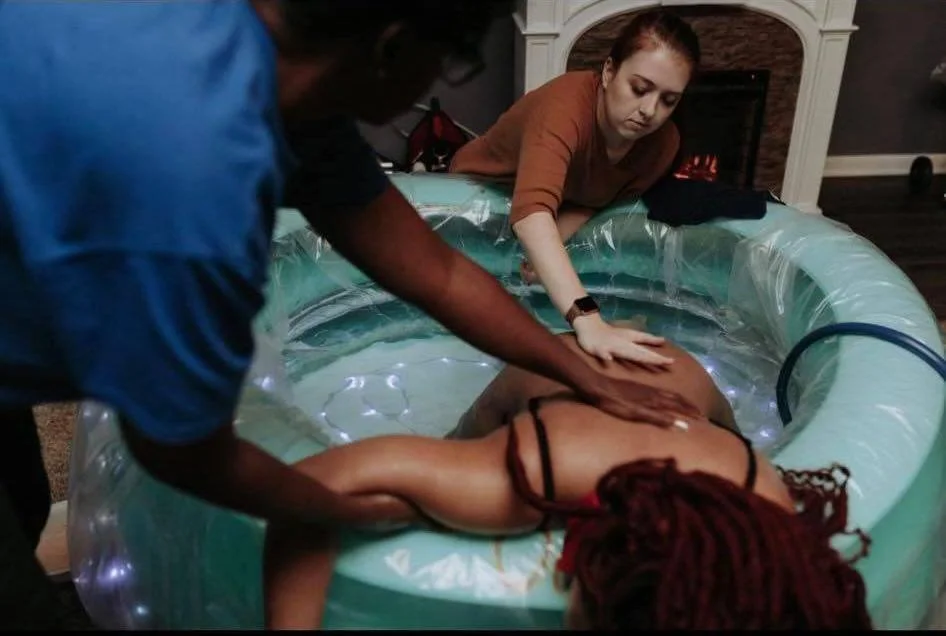
Essential Midwifery offers low-volume, personalized care for families seeking a more connected and intentional experience. Serving Marion County and surrounding areas, we provide home birth services along with comprehensive prenatal and postpartum care for low-risk women. By keeping our client load limited, we are able to offer attentive support, longer visits, and meaningful relationships that carry through every stage of care. Our approach blends clinical knowledge with a calm, supportive presence so you can feel confident, informed, and deeply cared for throughout your journey.
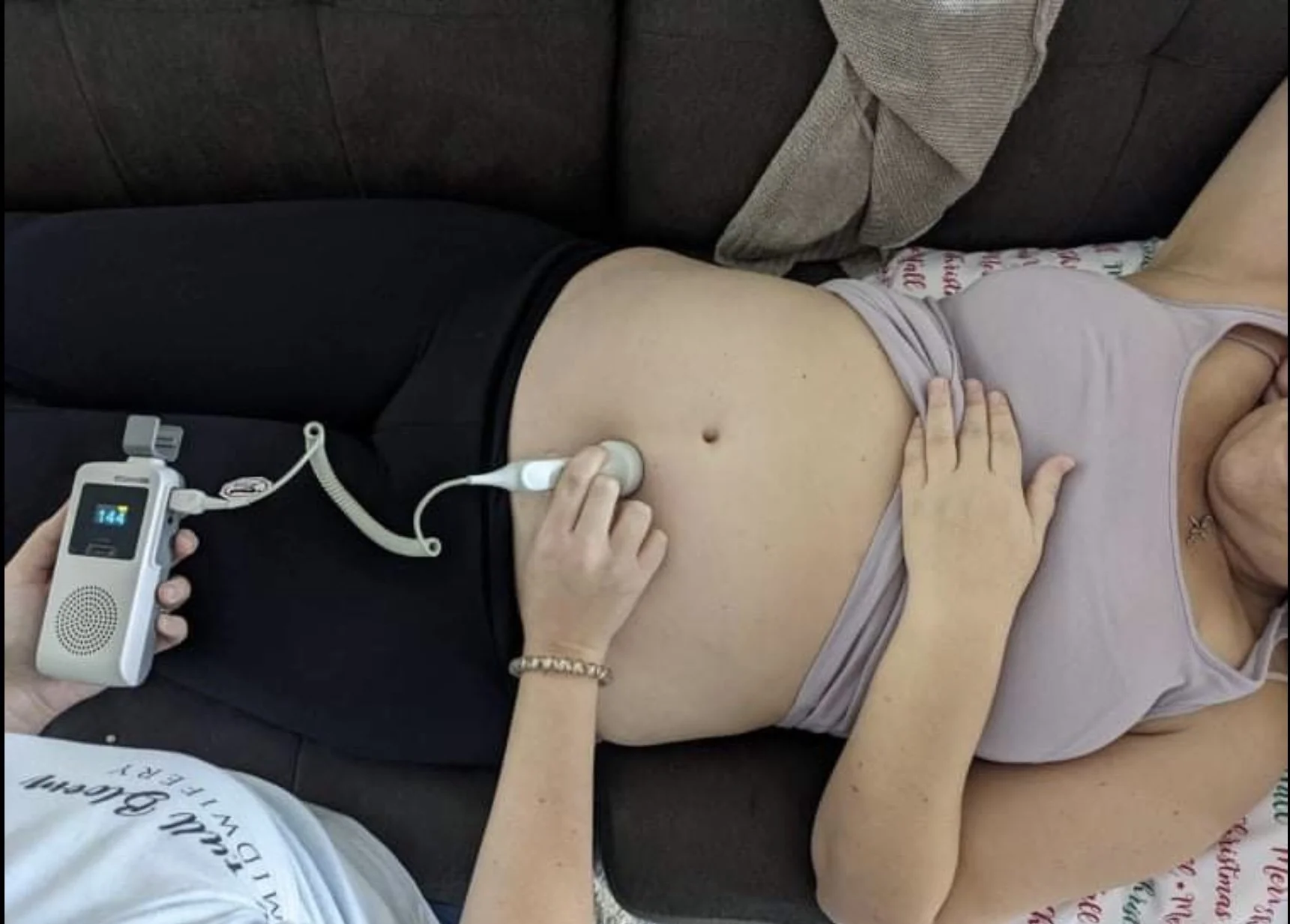
In-home prenatal care and home birth services.
Serving Marion County, FL and surrounding areas.
-
I am a licensed midwife with a deep passion for holistic care and natural birth. Caring for women and families is a calling I hold closely, and I am honored to serve my community with presence, respect, and heart.
-
Our approach is built on relationship, trust, and truly knowing the families we serve. We take time to listen, to support, and to walk with you through each stage of pregnancy, birth, and beyond with calm, intentional care.
-
Midwifery care is a good fit for families who desire a more personal, relationship based approach to pregnancy and birth. Those who value natural birth, informed choice, and a supportive, unhurried environment often find midwifery care to be a meaningful fit.